By Mel Bateson
 If you are anything like me, you may have noticed that there is increasing chatter about Gut Health in the mainstream media, recently. My first thought was of the stereotypical Dad with the rounded belly, the result of a lifetime imbibing food and beverage, and cleaning up his plate…to a fault. Turns out…yes and no, and so much more.
If you are anything like me, you may have noticed that there is increasing chatter about Gut Health in the mainstream media, recently. My first thought was of the stereotypical Dad with the rounded belly, the result of a lifetime imbibing food and beverage, and cleaning up his plate…to a fault. Turns out…yes and no, and so much more.
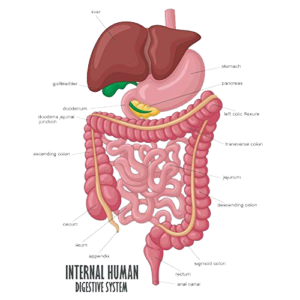
Anatomically, the gut is the segment of the gastrointestinal tract extending from the pyloric sphincter of the stomach to the anus and, as in other mammals, consists of two segments, the small intestine and the large intestine.
The gut is the ONLY organ that contains an intrinsic nervous system (Technically known as the enteric nervous system).
Interestingly the gut acts as a completely independent site of neural processing, which is why it is often called the SECOND BRAIN.
While this second brain is not believed to process conscious thoughts or decision-making, it does much more than merely handle digestion or gurgle when nervous. This little brain in our innards works hard, as we will discover in future posts. The Gut influences our immunity, mental health, detoxification, and hormones.
 What Does It Do?
What Does It Do?
The Gut, it turns out, has several functions. It:
- Digests our food
- Aids the production of certain vitamins, such as B and K
- Creates enzymes that destroys harmful bacteria
- Develops and maintains 80% of our immune function.
All systems in the body are intricately connected. It’s impossible to talk about gut health without discussing the connection between the immune system and the brain. The following fascinating facts, or FFF’s, will help you understand just how intimately intertwined the gut, brain, and immune system are:
- About 80 percent of the immune system is in the gut (in the gastrointestinal associated lymphatic tissue – known as GALT). Current research1 is increasingly teaching us about how the kind of bacteria, yeasts and parasites we have living in our gut affect how the immune system responds to different triggers, for example infectious agents or allergens.
- You have more neurons in your gut than you do in your brain. This collection of neurons is known as the enteric nervous system. It’s how you get ‘gut feelings’.
- You have more immune cells (microglia) in your gut than you have brain 2
Have a read of our blog Why Is Everyone Banging on about Gut Health? where we talk about the Gut-Brain Axis to better understand how when one system becomes taxed and compromised, other systems become severely strained and with time they begin to function poorly.
So, we now know that the gut is way smarter than we previously thought but what happens when this second brain starts to malfunction and I don’t mean an incidental brain fart (see what I did there 🙂 ) what happens to our health when our gut function is derailed?
This involves understanding terms such as dysbiosis, Leaky Gut and Microbiome (please see related blogs).
Dysbiosis is the general term used when the bacteria in the gastrointestinal tract is out of balance. By “out of balance”, we mean:
- When there are too many or too few microorganisms growing in the various sections of the gastrointestinal tract
- When the wrong kinds of microorganisms or the wrong balance between the different populations of microorganisms are present
A common form of gut dysbiosis is overgrowth of bacteria or yeast in the small intestine. This is referred to as small intestinal bacterial overgrowth, or SIBO. Catchy, huh.
Gut dysbiosis is strongly linked to chronic disease and has been found in every chronic disease in which a connection to gut bacteria has been investigated. Any of these circumstances can have profound impact on our digestion, gut barrier health, and the modulation of our immune systems. So what, I hear you mutter. Read on, friend, and prepare to be alarmed.
 2019 study, Baylor College of Medicine
2019 study, Baylor College of Medicine
A recent study took 41 females 12–17-year-old teenage girls participants who were medically healthy, non-medicated, in a major depressive episode or healthy controls, without any psychiatric condition, and compared the severity of the groups’ depressive symptoms, the activity of the autonomic nervous system, intestinal permeability, or gut leakiness, and the number of inflammatory cytokines. 3
The study found that:
- depression severity was associated with increased intestinal permeability
- the leakier the gut, the more severe the depression and depressive symptoms.
- the higher the concentration of the cytokine IL-1β, the more severe the depression.
- additionally, their evidence suggested that increased intestinal permeability may activate the innate immune system and push the development of depression.
I have to say, even given the small sample, the link seems quite clear.
Symptoms of Leaky Gut may manifest in a number of somewhat icky ways, and can include4:
- Upset stomach
- Constipation
- Diarrhea
- Bloating
- Nausea
- Bad breath
- Skin irritation or rashes
- Fatigue
- Brain fog
- Anxiety
- Depression
Gut dysbiosis doesn’t happen overnight. It’s much more likely that several dietary and lifestyle choices have led you to dysbiosis, as opposed to one major event, over time.
 Here are just a few causes of dysbiosis5:
Here are just a few causes of dysbiosis5:
- A diet high in processed carbs, sugar, and/or food additives
- Overuse of antibiotics
- Long-term prescription or over-the-counter drugs
- Drinking two or more alcoholic beverages per day
- Chronic stress, which can weaken digestion and your immune system.
So, dysbiosis, as well as making you feel pretty gross, can have far reaching, long term effects on your physical and mental health. All flatulence references aside, this is pretty serious stuff.
For further information please see:
Why Is Everyone Banging On About Gut Health
Is Your Gut Making You Feel Unhealthy, Paranoid, or Stressed Out?
References:
1.
Hsin-Jung Wu, Eric Wu. The role of gut microbiota in immune homeostasis and autoimmunity. Gut Microbes. 2012 Jan 1; 3(1): 4–14.
Yasmine Belkaid and Timothy Hand Role of the Microbiota in Immunity and inflammation Cell. 2014 Mar 27; 157(1): 121–141.
Gut Microbiome Dysbiosis and Immunometabolism: New Frontiers for Treatment of Metabolic Diseases. Mediators of Inflammation Volume 2018, Article ID 2037838, 12 pages
J. E. Belizario and M. Napolitano, “Human microbiomes and their roles in dysbiosis, common diseases, and novel therapeutic approaches,” Frontiers in Microbiology, vol. 6, p. 1050, 2015.
2.
Kathryn M. Lenz, Lars H. Nelson. Microglia and Beyond: Innate Immune Cells As Regulators of Brain Development and Behavioral Function. Front Immunol. 2018; 9: 698.
Zsuzsanna Szepesi, Oscar Manouchehrian et al. Bidirectional Microglia–Neuron Communication in Health and Disease. Front. Cell. Neurosci., 27 September 2018
3.
Calarge CA, Devaraj S, Shulman. Gut permeability and depressive symptom severity in unmedicated adolescents. J Affect Disord. 2019 Mar 1;246:586-594.
4, 5.
Simon Carding, Kristin Verbeke et al. Dysbiosis of the gut microbiota in disease. Microb Ecol Health Dis. 2015; 26: 10.3402/mehd.v26.26191.
Kamada N, Seo SU, Chen GY, Nunez G. Role of the gut microbiota in immunity and inflammatory disease. Nat Rev Immunol. 2013;13:321–35
Tanoue T, Umesaki Y, Honda K. Immune responses to gut microbiota-commensals and pathogens. Gut Microbes. 2010;1:224–33.